What is Angina?
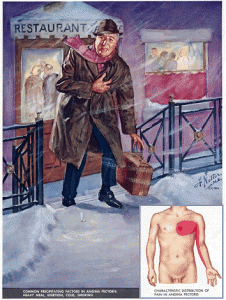
The arteries which supply the heart muscle with oxygen (the coronary arteries) do so by delivering oxygenated blood to the heart muscle (myocardium). Healthy coronary arteries can deliver increased blood flow when the heart muscle demands it. If however there is a narrowing or blockage in one or more of the coronary arteries, the demand for increased oxygen or blood at certain times cannot be met due to the fixed restriction to blood flow caused by the narrowing or blockage in the artery.
Angina is the symptom experienced by the patient when the demand of the heart muscle exceeds the supply of oxygenated blood.
Symptoms
The literal Latin translation of the word angina is “choking” as Angina is often experienced by the patient as a tight or squeezing feeling in the upper portion of the chest and may radiate to the throat. Some patients experience genuine pain, most typically in the centre of the chest, with some spread or radiation to both sides. Pain may also radiate to the neck or jaw and down both arms or one arm. For some patients the experience is that of tightness rather than pain and some patients do not actually experience chest discomfort at all. The absence of pain is particularly common in the elderly population and in those with diabetes. For some patients breathlessness may be the only symptom experienced.
Causes of Angina
The most common cardiac risk factors in western societies include cigarette smoking, diabetes, high blood pressure, high cholesterol, obesity and lack of exercise. The distribution of excess weight is also an important factor with abdominal obesity carrying the greatest risk. A family history of premature coronary artery disease also adds to the individual risk.
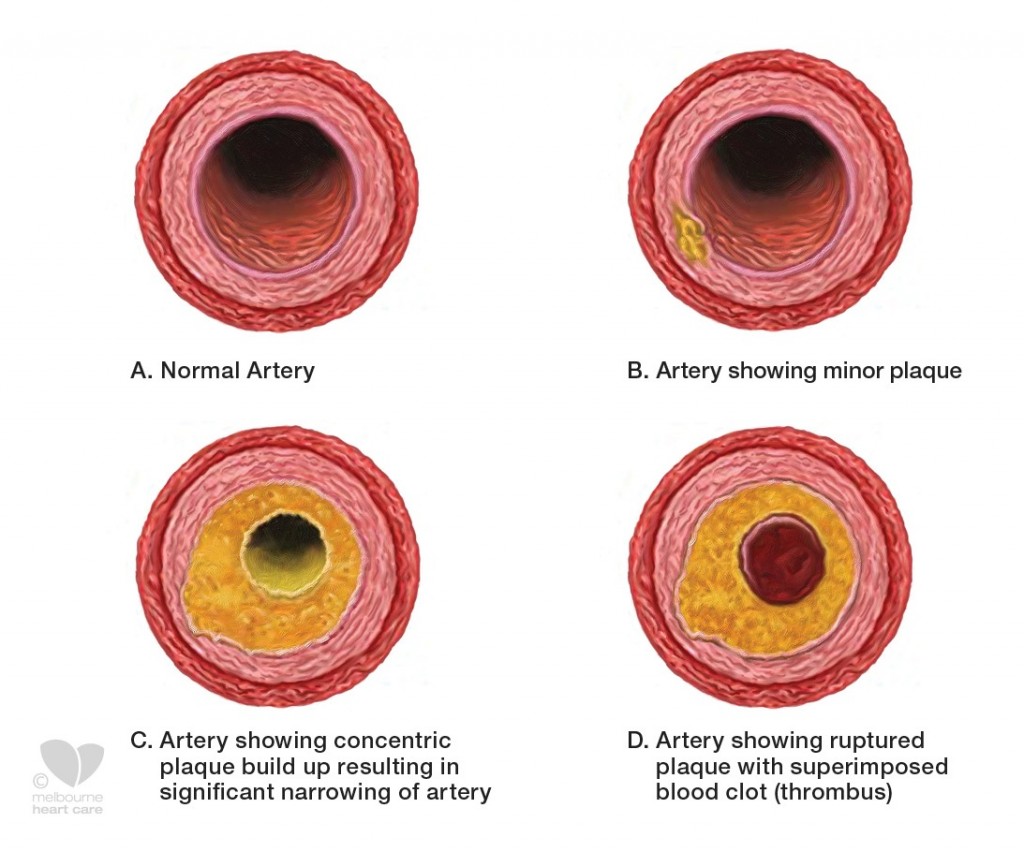
If the coronary arteries become too narrow then the blood supply to the heart muscle can be reduced. Patients are most likely to experience Angina when the heart’s demand for oxygen is increased, for example during physical exertion or emotional stress. However as the severity of the narrowing in the coronary artery worsens then symptoms can become more unstable with Angina occurring at rest or even during the night.
Typically however, Angina is more likely to occur during physical activity and for many patients is more likely in cold conditions or after a heavy meal.
Other Causes of Angina
Some patients experience Angina due to “spasm” of the coronary arteries. This condition, often referred to as variant or Prinzmetal Angina, is more common in women, the younger population, and is more likely to occur at rest rather than during physical activity.
In this form of Angina the wall of the coronary artery may actually contain no build-up of atheroma or only a small or minor plaque. Intermittently however the coronary artery, which is a muscular structure, contracts or goes into spasm which transiently reduces the blood flow through the vessel.
This can result in typical Angina-like symptoms which usually respond to appropriate medication (see Therapy for Angina).
Diagnosis
By far the most important step in the diagnosis of this condition is to seek medical assistance and describe your symptoms to your doctor.
It is extremely common for patients to mistake their symptoms for heartburn and thus delay seeking medical advice.
If your doctor feels that you may have Angina, a number of tests may be ordered to facilitate the diagnosis including an electrocardiogram (ECG), exercise stress test, exercise stress echocardiogram, CT coronary angiogram or coronary angiogram (see Diagnostic Tests and Procedures).
Treatment
It is vitally important for all patients diagnosed with coronary artery disease to pay attention to lifestyle factors which may be placing them at risk, for example cigarette smoking.
Your physician will encourage you and assist you in making healthier lifestyle choices which will help to reduce future risk.
These lifestyle changes may include quitting smoking, reducing weight, implementing an appropriate exercise program as well as appropriate dietary changes.
Along with appropriate lifestyle modification, patients may require medications with or without the need for a mechanical intervention such as coronary angioplasty and stenting or coronary artery bypass graft surgery.
Medications
Some medications prescribed by your physician are designed to relieve symptoms and others are targeted towards reducing the risk of future cardiac events such as heart attack.
Aspirin
A daily low dose of Aspirin is indicated for the vast majority of patients with diagnosed coronary artery disease. Aspirin is used to ‘thin the blood’. Aspirin acts to reduce the stickiness of one of the components in our blood stream responsible for blood clotting (platelets). Thus patients who take Aspirin are less likely to form a blood clot within one of the coronary arteries.
Statins
Statins are a class of cholesterol-lowering medications which act by inhibiting the enzyme HMG-CoA reductase. They result in a lowering of the blood cholesterol levels, however they also have the additional property of stabilising the cholesterol plaques or atheroma within the wall of the coronary circulation.
An important component of treatment of the patient with atherosclerosis is to minimise the risk of plaque rupture and this class of medication has been proven to substantially reduce the risk of this occurrence.
Nitrates
Short-Acting Nitrates: Short-acting nitrate medications can be a spray or a tablet administered under your tongue. The most common form is GTN or glycerol trinitrate. This medication is used to relieve the symptom of angina and acts rapidly.
This kind of medication is used as required or when you experience symptoms and thus should be carried with you at all times.
Long-Acting Nitrates: Long-acting nitrates may be provided in a topical form such as GTN patches or a longer-acting oral form via a tablet, which is swallowed. These forms of therapy provide a slow and continuous release of the active nitrate substance into the bloodstream, thus helping to prevent episodes of angina.
It is important with long-acting nitrates for the body to have a nitrate-free period so that you do not build up a tolerance to the medication making it ineffective. Thus the patch would only be applied for 12 hours per day, using a fresh patch each day applied to a different area of the skin.
Important Note
Short-acting Angina medication can lose its effect if not stored properly.
Tablets should be stored in their original glass container and protected from moisture, light and heat.
Do not throw out the cottonwool-like substance in the top of the container because it stops the tablets deteriorating.
Don’t carry tablets too close to your body as the heat of your body can make the medication deteriorate.
Renew your medication three months after you open the bottle.
Anginine tablets can be purchased over the counter in Australia and do not require repeat prescription.
Beta-blockers
Beta-blockers reduce Angina by reducing heart rate and blood pressure and thus the oxygen demand of the heart, particularly during times of stress or exertion.
The most common side effect of beta-blockers is that of fatigue, however often this effect can lessen as your body becomes more familiar with the medication. Other common side effects can include sleep disturbance, lowered mood and erectile dysfunction. You should consult your physician if you are experiencing adverse side effects.
Calcium channel blockers
Calcium channel blockers are also often effective for treatment of anginal symptoms. They act via dilating the coronary arteries and improving the blood flow to the heart muscle or reducing the heart rate and thus the heart muscle’s demand for oxygen.
Other Medications
Other more recently developed angina medications include Nicorandil (Ikorel) and Ivabradine (Coralan).
Many patients with angina require a combination of the above-mentioned medications in order to appropriately control their symptoms, reduce their risk and improve their quality of life.
Mechanical or Surgical Treatments
Coronary angioplasty
Coronary angioplasty and stenting is a relatively common procedure used for the treatment of Angina. During coronary angioplasty a small balloon is inflated inside one or more of your coronary arteries to open up the narrowed area and improve the blood flow through the vessel.
In the majority of cases a flexible expandable metal tube (a stent) is placed within the narrowing and expanded to keep this area of the artery widely open. Angioplasty is performed under local anaesthetic where a small tube is placed into either the radial artery in the wrist or the femoral artery in the groin.
Most patients can be discharged from hospital the day after their angioplasty and stenting procedure.
Coronary Artery Bypass Graft Surgery
Coronary artery bypass graft surgery is performed when the narrowings in the coronary arteries are not suitable for angioplasty and stenting or it is felt that the patient will achieve a better overall result with bypass grafting.
Coronary Artery Bypass Graft surgery (CABG) is an operation performed under general anaesthetic where a blood vessel, or blood vessels, are taken from your chest, forearm or leg and grafted to your coronary artery beyond the narrowing to bypass the problematic area. This improves blood flow to the heart muscle and usually results in a significant reduction in Angina symptoms.
Warning Signs
For many patients the pattern of their angina remains relatively stable, for example,symptoms only occurs when walking uphill.
If, however, you notice that your pattern of Angina is changing you should notify your physician.
You should talk to your doctor if your Angina:
- Becomes more severe
- Is occurring more frequently
- Is lasting longer
- Doesn’t respond as well to medicine such as nitrates
- Is occurring with less exertion or at rest
- Is occurring at night
If your episode of Angina is not relieved with usual treatment such as rest or use of your nitrate medication, you could be having a heart attack and you should call 000 immediately and ask for an ambulance.
